The dangers of nursing home neglect
 We place trust in nursing homes to care for our elders. But unfortunately, nursing home neglect is far too common, resulting in numerous health complications and deaths in Georgia and nationwide. It only takes a little carelessness or lack of experience to put our elders at risk.
We place trust in nursing homes to care for our elders. But unfortunately, nursing home neglect is far too common, resulting in numerous health complications and deaths in Georgia and nationwide. It only takes a little carelessness or lack of experience to put our elders at risk.
When a resident doesn’t receive an adequate level of care in a nursing home, serious health issues can develop. That’s why it is the responsibility of nursing homes to promote hygiene, sanitary conditions, safety, and mobility. Nursing home staff are expected to help residents maintain hygiene and a healthy diet, change bedding positions, walk and exercise. This helps residents sustain healthy circulation, balance, strength and overall well-being. But unfortunately, not all nursing home staff are as attentive as they should be.
What are pressure sores?
In far too many cases, residents are left unattended in beds and wheelchairs. For residents who are unable to perform physical activities, lack of mobility can result in serious health issues. Some of the most common are pressure sores (also known as bed sores and pressure ulcers), which occur when the skin and underlying tissue begin to break down. When a patient has been lying in bed or sitting in a stationary position for a prolonged period of time, blood circulation and oxygen gets cut off from the affected area, resulting in tissue damage and cell death.
Pressure sores typically occur in areas where there is little connective tissue separating the skin and bones, such as the ankles, elbows, heels, knees, and hips. Pressure sores are often diagnosed by their size, shape, and amount of fluid discharge. which doctors can use to determine the stage and decide which treatment would be appropriate. Most pressure sores can be healed with proper treatment, especially if they only affect the outer layers of skin. But prolonged neglect can lead to more serious pressure sores that can prove to be fatal.
Primarliy residents over the age of 70 are at risk of developing pressure sores. This is in part due to thinning, drier skin with less elasticity. The skin and connective tissue break down quickly and heal slowly. Obesity is also a significant risk factor for pressure sores, as extra weight can cut off circulation to the affected area. Other risk factors include diabetes, poor nutrition or a history of cigarette smoking.
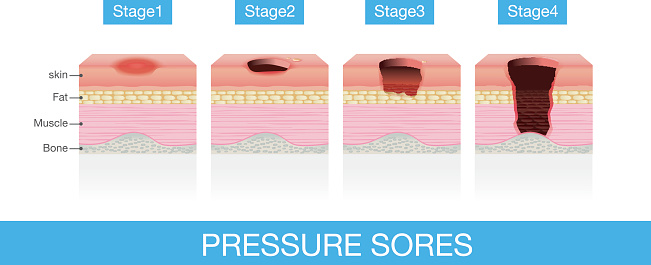
Stages of Pressure Sores
How serious are pressure sores?
Pressure sores are classified into four stages - ranging from mild (Stage I) to severe (Stage IV). While Stage I and Stage II tend to be relatively easily treated, serious health complications can result from Stage III and Stage IV. Stage III pressure sores occur when an ulcer grows beyond the second layer of the skin, corroding its way into fat tissue. This type of pressure sore often appears in the shape of a crater and may be accompanied by a foul odor. Stage IV is the most severe type of pressure sore, growing beyond fat tissue and affecting muscles, ligaments, tendons, and bones. These pressure sores will often leave underlying connective tissue exposed, and if untreated, can lead to blood poisoning and bone infections.
Patients suffering from Stage III and Stage IV pressure sores can develop a life-threatening condition called sepsis. This occurs when the infection from the pressure sore causes the bloodstream to become flooded with bacteria. In response, chemicals from the immune system are released to fight the infection, but instead end up causing severe inflammation, damaging vital organs. Often, a patient’s blood pressure drops to dangerous levels, which threatens the heart, kidney and lungs, leading to septic shock and potentially death.
What can be done?
In nursing homes and assisted living facilities, pressure sores are always preventable. By keeping skin clean and dry, changing positions every two hours and using cushioned surfaces, caregivers can prevent pressure sores from forming. A healthy diet comprised of an adequate amount of protein and fluids can keep the skin and connective tissue intact. Moreover, regular body checks can catch pressure sores early, while they are still in Stage I or Stage II and can generally be treated via minimally invasive means.
Stage III and Stage IV pressure sores can be treated as well, but the process is much more difficult, painful and costly. Doctors may have to remove infected tissue in order to prevent the sore from spreading. Antibiotics may also be prescribed in order to fight infection.
Unfortunately, when nursing homes are short-staffed or have inexperienced or untrained staff, pressure sores can be allowed to fester, with serious and potentially fatal consequences. If your loved one has developed a pressure sore due to nursing home neglect, it is important that you speak with an attorney who knows how to handle these cases. Nursing homes and their staffs should be held accountable if their negligence results in a resident developing pressure sores.
Sources:
- American Academy of Family Physicians (2017). Pressure Sores. – via familydoctor.org.
- Medline Plus (2016). How to Care for Pressure Sores. – via medlineplus.gov.
- Medical News Today (2017). Sepsis: What You Need to Know. – via medicalnewstoday.com.
